Articles
- Page Path
- HOME > STRESS > Volume 25(2); 2017 > Article
-
Review Article
정신건강문제를 중재한 수용전념치료 연구에 대한 통합적 문헌고찰 - 최덕자, 김성재
- An Integrative Review of Acceptance and Commitment Therapy (ACT) for Mental Health Problem
- Dugja Choi, Sungjae Kim
-
Korean Journal of Stress Research 2017;25(2):75-85.
DOI: https://doi.org/10.17547/kjsr.2017.25.2.75
Published online: June 30, 2017
서울대학교병원 간호부문
서울대학교 간호대학 간호과학연구소
Department of Nursing, Seoul National University Hospital, Seoul, Korea
The Research Institute of Nursing Science, College of Nursing, Seoul National University, Seoul, Korea
- Corresponding author Sungjae Kim College of Nursing, Seoul National University, 103 Daehak-ro, Jongno-gu, Seoul 03080, Korea Tel: +82-2-740-8814 Fax: +82-2-765-4103 E-mail: sungjae@snu.ac.kr
Copyright: © The Korean Journal of Stress Research
This is an open access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 2,165 Views
- 105 Download
- 9 Crossref
Abstract
- 본 연구는 국내 수용전념치료 연구를 통합적으로 고찰하여 치료의 효과성과 임상적 유용성을 파악하고, 이를 근거로 향후 연구 방향과 효과적인 프로그램 구성 및 전략을 제시하고자 시도하였다. 연구결과, 대상자의 특성과 연구 목적에 따라 수용전념치료의 6가지 핵심 원리를 유연하게 구성하는 것이 중요 전략임을 확인하였다. 즉, 불안은 기꺼이 경험하기와 인지적 탈융합을 강조하고, 우울은 자기자비와 자기수용에 초점을 두며, 중독은 비효과적인 대처 감소를 위해 전념행동에 중점을 두고, PTSD는 현재에 존재하기에 역점을 두어 중재하는 것이 효과적이었다. 수용전념치료는 저항적이고 만성화 경향이 있는 정신건강문제에 효과적인 중재가 될 수 있으므로, 조현병이나 양극성 장애를 위한 수용전념치료 프로그램의 개발이 필요하다.
Abstract
- The purpose of this study was to provide an integrative review of ACT for mental health problems to identify content of program and discuss methodological strategy of intervention according to target population. According to Whittmore and Knaf’s integrative review method, this research was conducted in five stages: clarification of research problems, literature search, and quality evaluation of data, data analysis, and data description. The key words in English and Korean were used to search through seven electronic databases. 21 studies were finally included in this integrative review. ACT was used as an intervention for anxiety, depression, posttraumatic stress disorder and eating disorders and was effective in social avoidance, anxiety sensitivity, depression, dysfunctional belief and negative thinking. It was also used as an intervention for the maladjustment in adolescence to improve self-esteem and reduce behavioral problem. The six core processes of ACT are useful for people with chronic mental illness who have an ineffective avoidance strategy that avoids their symptoms and does not accept the illness. We give a suggestion that researchers develop and apply appropriate ACT for mentally ill person in hospitals.
- Keywords: Mental health, Mentally ill person, Acceptance and Commitment Therapy (ACT)
- 우리나라 정신장애 평생 유병률은 2006년 12.3%에서 2011년 14.4%로 증가하였다(Cho MJ et al., 2012). 이는 사회구조가 복잡해짐에 따라 가족, 학교, 직장 등 사회전반에 걸쳐 갈등이 증가하였고, 그로 인해 학교 폭력 및 왕따 현상, 게임 중독, 이혼 등 심각한 사회문제가 발생하면서 우울증이나 다양한 정신건강문제가 증가되는 것으로 생각된다(Lee SY, 2013). 이러한 정신건강문제는 조기 치료와 중재가 제대로 이루어질 경우에는 예후가 좋으나 잘 관리되지 않을 경우 반복되는 재발을 일으키며 만성적인 정신질환으로 진행하게 된다.
- 정신건강문제를 조기에 중재하기 위해 약물치료와 정신재활치료는 매우 중요하며 이는 증상의 악화와 재발에 매우 밀접한 관계를 가지고 있다. 특히 약물치료는 급성기 증상을 감소시키며 정신건강문제를 중재하는 가장 빠르고 효율적인 방법으로 제시되어 왔다(Jin HK et al., 2016). 그럼에도 불구하고 대부분의 대상자는 약물부작용과 사회평가에 대한 두려움으로 치료를 회피하려는 경향이 많으며(Jimenez et al., 2013), 치료를 시작한다고 하더라도 본인의 의지보다는 가족이나 타인에 의해 시작하는 경우가 많아 치료 순응도가 매우 낮다(Jin HK et al., 2016). 따라서 대상자들의 치료 순응도를 높이기 위해서는 자신의 병을 수용하고 자발적 동기를 바탕으로 적절한 치료적 중재를 받아들일 수 있는 접근이 매우 필요하다. 또한 정신재활치료는 대상자가 독립적이며 효율적인 기능으로 사회생활을 할 수 있도록 도와주기 때문에 약물치료와 병행하는 것이 바람직하다(Lee OJ et al., 2004). 정신재활치료에는 대상자의 내적 갈등과 어려움을 들어주고 지지해주는 지지정신치료, 역기능적인 사고와 행동에 대한 인지오류를 수정하도록 돕는 인지행동치료, 가족에게 질병과 치료에 대한 교육과 가족역동의 문제를 확인하고 해결하도록 돕는 가족치료, 사회 생활하는데 필요한 다양한 기술을 배우고 훈련하는 사회기술훈련, 질병의 증상과 약물에 대한 지식을 제공하는 정신교육과 같은 다양한 프로그램이 있다. 그러나 이와 같은 정신재활 프로그램은 대부분이 자기 자신이나 질병에 대한 수용 없이 프로그램에 참여하기 때문에 증상을 일시적으로 감소시키는 효과는 있으나 재발률 감소에는 효과적이지 않는 것으로 보고되고 있다(Kingston, 2008). 이는 대상자가 자발적 동기 없이 수동적으로 참여하는 경우에 장기적 효과는 제한적일 것이라고 해석할 수 있다(Johansson et al., 2006). 이처럼 약물치료와 정신재활치료 모두 환자의 정신건강문제를 해결하기 위하여 요구되는 중요한 프로그램이지만, 치료 원리와 접근방식의 대부분이 대상자가 스스로 자신의 행동 방식을 선택하기 보다는, 치료자가 바람직한 방향과 방법으로 의 변화를 제시하는 접근 방식이기 때문에, 대상자의 역할은 매우 수동적이 된다는 한계가 있다(Johansson et al., 2006; Jin HK et al., 2016). 대상자가 보다 적극적이고 능동적으로 치료에 참여하기 위해서는, 증상 완화와 행동변화 교육에 초점을 두는 치료자 중심의 접근법보다는, 자신의 경험을 회피하지 않고 수용함으로써 진정으로 자신이 원하는 가치를 깨닫고 상황에 효과적으로 대처할 수 있도록 돕는 대상자 중심의 접근법이 매우 효과적일 것이다(Jung HK, 2004). 이러한 접근법으로는 인지치료의 제3동향의 하나인 수용전념치료(Acceptance and Commitment Therapy: ACT), 마음 챙김 기반 스트레스 감소 프로그램(Mindfulness Based Stress Reduction: MBSR) 및 마음챙김 인지치료(Mindfulness Based Cognitive Therapy: MBCT)가 대표적이다(Moon HM, 2005). 그 중 수용전념치료는 새로운 형태의 인지행동치료로서 인지나 정서의 내용에 대한 변화를 추구하는 기존의 중재와는 달리, 자기수용을 통해 진정한 삶의 가치를 찾아 실현하도록 돕는 것을 목적으로 한다(Bach et al., 2002). 이는 고통을 통제하거나 경험을 회피하는 전략이 오히려 문제해결을 어렵게 만든다는 것을 지적하고, 통제나 회피보다 현재의 순간에서 있는 그대로 경험하여 이해를 증진시키도록 돕는다(Bach et al., 2002). 수용전념치료에서 심리적 건강의 핵심 지표로 보는 심리적 유연성은 변화하는 환경요구에 대한 불필요한 방어 없이 자신이 경험하는 생각과 감정 그리고 신체감각들에 충분히 접촉하면서, 더불어 가치 추구를 위한 행동에 전념하는 능력으로 정의된다(Eifert et al., 2009). 수용전념치료에서 심리적 유연성을 기르는 것은 고통의 통제와 회피에서 벗어나 기꺼이 경험하도록 도와주며 자신의 가치를 찾아 자유로운 선택을 할 수 있게 돕는다(Kingston, 2008). 특히 정신건강문제에 부정적이고 회피적인 동양인들에게는 증상완화를 하기 위해서 치료자가 주도하에 인지나 정서의 직접적인 변화를 추구하는 방법보다는 스스로 자신의 상태를 수용하고 자신이 변화의 주체가 되도록 유도하는 수용중심의 접근법이 효과적일 것이라고 생각한다.
- 1990년대 후반부터 외국에서는 우울이나 불안, 조현병과 같은 다양한 정신질환 대상자들에게 적용한 수용전념치료의 효과가 보고되었으며(Powers et al., 2009), 축적된 연구들의 메타분석을 통해 그 효과의 근거를 보고하고 있다(Davis et al., 2015). 국내에서는 2010년부터 시험불안 학생을 대상으로 중재한 연구를 시작으로 수용전념치료를 적용한 논문이 학술지에 보고 되기 시작하였다(Hwang SO et al., 2010). 이렇게 수용전념치료에 대한 관심이 증가하면서 그 효과를 보고하는 연구결과들이 지속적으로 발표되고는 있으나, 국내에서 시행한 수용전념치료에 대한 통합적 고찰은 이뤄지지 않고 있는 실정이다. 수용전념치료에서는 문화적 맥락을 이해하고 가치를 추구하는 것이 매우 중요한 부분이므로, 문화적 차이가 있는 외국의 근거자료를 그대로 적용하는 것은 무리가 있다고 본다. 이에 본 연구는 정신건강문제에 따른 효과적인 수용전념치료를 개발하고 적용하기 위한 근거 자료를 마련하기 위하여, 통합적 문헌고찰 방법을 통해 국내에서 수행된 연구들에서 사용한 수용전념치료의 진행방식, 중재내용, 적용대상 및 효과를 파악하고자 한다. 그리고 이를 바탕으로 주요정신질환 중 하나인 조현병과 양극성장애에 적용 할 수 있는 중재전략을 제시하고자 한다.
서론
- 1. 연구 설계
- 본 연구는 최근 국내에서 수행한 수용전념치료 중재 연구를 통합적으로 고찰하여 다양한 정신건강 문제를 지닌 대상자에게 적용할 수 있는 효과적인 수용전념치료 개발을 위한 근거자료를 제시하고자 시도된 통합적 문헌고찰이다. Whittemore et al.(2005)이 제시한 통합적 문헌고찰 지침에 따라 연구 문제의 명료화, 문헌 검색, 자료의 질 평가, 자료 분석 및 자료 기술의 5단계로 연구를 진행하였다.
- 2. 연구 대상
- 분석대상 논문의 선정기준 Cochrane Collaboration에서 널리 사용하는 PICO (Population, Intervention, Comparisons, Outcomes)틀에 근거하였다. 본 연구의 대상자(Population)는 13세 이상의 청소년과 성인을 대상으로 한 연구이며, 중재(intervention)는 수용전념치료를 선택한 연구이며 대조군(comparison)으로 중재를 받지 않거나 수용전념치료 외 다른 치료를 받은 대조군이 있는 연구이며, 결과(outcome)는 통계적으로 유의한 변화가 있는 결과변수를 한 개 이상 포함하고 있는 논문으로 선정하였다.
- 3. 자료수집
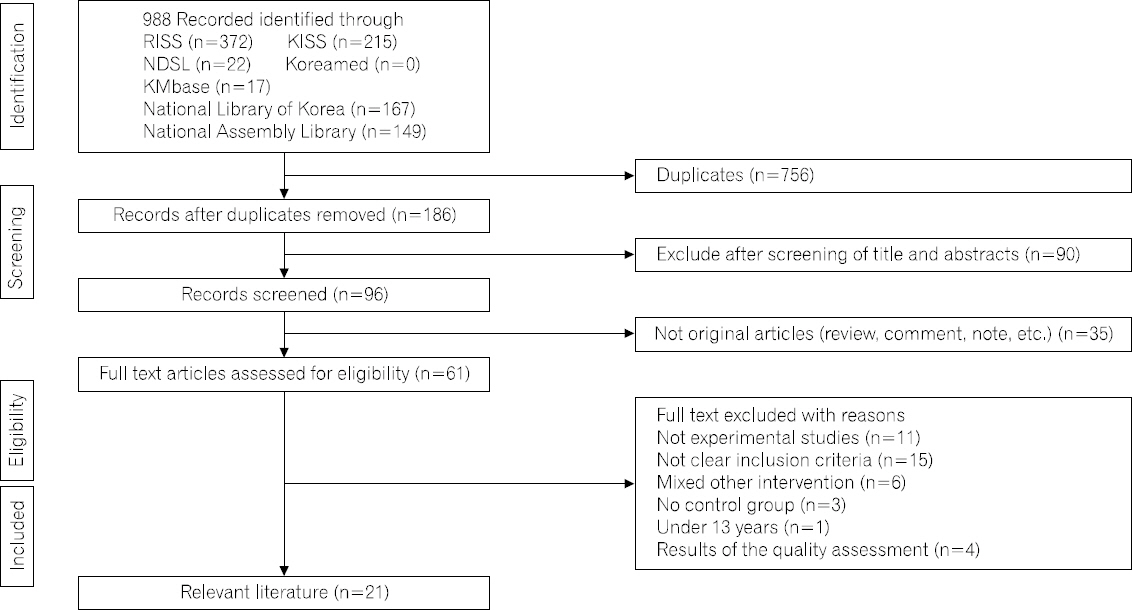
- 본 검색을 시작하기 전에 일차적으로 근거기반간호의 임상질문 양식인 Population (P), Intervention (I), Comparison (C), Outcome (O) (PICO)을 기반으로 검색어를 “수용전념치료”, “수용전념중재”, “수용전념” 및 “Acceptance and commitment therapy”로 결정하였다. 문헌 검색기간은 2017년 1월 15일부터 2017년 1월 21일까지였으며, 코리아메드, 국립중앙도서관, 한국학술정보, 국가과학기술정보센터, 국회도서관, 한국교육학술정보원의 학술연구정보서비스 및 한국의학논문 데이터베이스 등 총 7개의 인터넷 검색 데이터베이스를 이용하여 검색하였다. 단, 국내 데이터베이스의 경우 문헌검색의 민감도와 특이도를 고려했을 때 검색에 제약이 있어, 이 검색어를 이용하여 폭넓게 검색한 후 직접 수기로 선별하였다. 자료 수집과 선별의 전 과정은 수용전념치료에 대해 전문적인 교육훈련을 받은 2명의 연구자가 모든 연구들을 독립적으로 검토하여 선택하였다. 위 문헌검색 전략에 의해 검색된 문헌은 942편이었다. 중복문헌 756편을 일차적으로 제외하였다. 그 외에 수용전념치료가 아닌 연구 90편, 학위논문, 종설, 학술대회자료집 등 원저가 아닌 경우 35편, 비실험 연구 11편, 수용전념치료와 다른 치료 프로그램을 혼용하여 중재한 연구 6편, 대조군이 없는 단일실험 연구 3편, 13세 이하의 아동을 대상으로 한 연구 1편, 대상자 선정기준이 명확하지 않은 대상자를 연구대상으로 한 연구 15편을 제외하고 25편의 연구가 선정되었다. 두 연구자가 질 평가를 하면서 연구도구 해석의 문제가 있는 연구 4편이 있어 저자에게 직접 메일로 문의하였으나 응답이 없었다. 질의에 응답이 없는 이 4편의 연구를 용인할 수 없는 수준(unacceptable-reject)으로 평가하여 최종적으로 고찰대상 문헌에서 제외하여 최종적으로 선택한 문헌은 총 21편이었다(Fig. 1).
- SIGN은 세계적으로 많이 사용되고 있고 연구의 질에 대해 가장 포괄적 평가가 가능하며 RCT연구뿐만 아니라 Non-RCT 연구와 질적 연구 등 다양한 연구방법에 대한 질 평가가 가능하도록 만들어진 평가도구이다(SIGN., 2015). 따라서 본 연구에서는 연구 설계를 명확하게 결정하기 위해 SIGN을 이용하여 질 평가를 수행하였다. 질 평가는 연구자 2명이 해당 연구들을 독립적으로 평가한 후 두 평가자간 결과를 확인하였으며 이견이 있는 경우 두 평가자가 논의 후 합의를 이루는 결과로 결정하였다. SIGN의 기준에 따라 무작위임상연구가 아닌 경우에는 무작위배정, 은닉, 맹검 문항을 no로 평가하고, 근거수준을 수용 가능한 정도 (acceptable, +), 낮은 정도(low quality 0), 용인할 수 없는 수준(unacceptable- reject)으로 평가하였다(Table 1).
- Quality assessment of the selected studies, following the SIGN methodology checklist
연구방법
| Authors (year) | Study design | Level of evidence | Clear purposes statement | Random assignment | Allocation concealment | Blind about treatment allocation | Homogeneous test | Difference between group is only treatment | Standard, valid and reliable measurement for outcomes | Drop-out rate (%) | Intention to treat analysis |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Kim & Kim (2012) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 18% | No |
| Kim & Son (2013) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 10% | No |
| Kim & Back (2013) | Non-RCT | 0 | Yes | No | No | No | Yes | Yes | Yes | 18% | No |
| Kwon & Chung (2014) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 12% | No |
| Ko & Kim (2015) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 9% | No |
| Kim & Son (2016) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 0% | No |
| Kim & Son (2013)* | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 10% | No |
| Lee & An (2012) | Non-RCT | 0 | Yes | No | No | No | Yes | Yes | Yes | 10% | No |
| Yang & Shin (2013) | Non-RCT | 0 | Yes | No | No | No | Yes | Yes | Yes | 44% | Yes |
| Kim & Park (2014) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 4% | No |
| Ha & Son (2016) | Non-RCT | 0 | Yes | No | No | No | Yes | Yes | Yes | Can’t say | Can’t say |
| Yu & Son (2016) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | Can’t say | Can’t say |
| Joh & Son (2013) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | Can’t say | Can’t say |
| Lee & Son (2013) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | Can’t say | Can’t say |
| Jung & Lee (2014) | Non-RCT | 0 | Yes | No | No | No | Yes | Yes | Yes | 20% | No |
| Seo & Kim (2012) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 10% | No |
| Noh & Son (2014) | RCT | 1+ | Yes | Yes | Yes | Can’t say | Yes | Yes | Yes | 16% | No |
| Ju & Son (2015) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 25% | No |
| Choi & Son (2011) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 25% | No |
| Song & Son (2011) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 13% | No |
| Jang & Son (2012) | RCT | 1+ | Yes | Yes | Can’t say | Can’t say | Yes | Yes | Yes | 22% | No |
- 1. 연구 자료의 일반적인 특성 및 질 평가
- 본 연구에서 최종 선택된 연구 21편의 일반적인 특성은 다음과 같다. 연구 논문이 출판된 시기는 모두 2010년 이후였고 2011∼2013년 사이에 12편(57.1%) 그리고 2014∼2016년 9편(42.9%)이 보고되었다. 연구 설계는 무작위 실험 연구가 16편(76.2%)으로 가장 많았고 유사 실험연구 5편(23.8%)이 있었다. 주요 연구대상은 불안 8편(38.1%), 우울 2편(9.5%), 중독 5편(23.8%), 외상 후 스트레스 장애 3편(14.3%), 신체상 장애 2편(9.5%) 그리고 학교부적응 1편(4.8%)으로 나타났다. SIGN의 알고리즘에 따른 문헌의 질 평가 결과는 Table 1과 같다. 21편의 논문은 모두 연구 질문에 대해 명확하고 적절하게 기술하였다고 평가된다. 연구설계 중 무작위 할당에 대한 평가 결과는 1편에서만 컴퓨터 코딩을 이용한 무작위 할당을 하였음을 구체적으로 언급하였고 그 외 15편의 논문에서는 무작위 할당 방법에 대한 구체적인 방법을 기술하지 않았다. 또한 21편 모두 중재의 은폐나 중재에 대한 가림, 그리고 이중 맹검의 실시여부에 대한 언급이 전혀 없었다. 4편의 연구에서는 탈락률을 언급을 하지 않았고 1편의 연구에서는 탈락률이 44%로 매우 높아 낮은 평가를 받았으며 나머지 16편의 연구에서는 탈락률이 25% 미만으로 나왔다. 각 항목에서 두 연구자 간의 합의하에 ‘그렇다’로 평가된 수가 7개 이상일 때 높은 질(high quality, 2+)로 평가하고 5개∼6개이면 근거 수준을 수용 가능한 정도(acceptable, 1+), 4개일 때는 낮은 정도(low quality, 0), 3개 이하인 경우는 용인할 수 없는 수준(unacceptable-reject)으로 평가하였다. 수용 가능한 정도의 수준은 16편 그리고 질적으로 낮은 수준의 연구는 5편이었다.
- 2. 수용전념치료 중재 분석
- 한 회기당 중재시간이 90∼120분인 연구가 19편(90.5%), 60분이 2편(9.5%)이었다. 중재기간을 살펴보면 주 2회씩 4∼5주간으로 구성된 프로그램을 적용한 연구가 11편(52.4%), 주 1회씩 8∼10주간으로 구성된 연구가 8편(38.1%)이었으며, 2편은 중재기간을 정확하게 명시하지 않았다. 중재 후 사후 추적조사를 실시한 연구는 16편(76.2%)이었고, 16편 중, 중재 4주 후에 추적 조사를 한 논문은 7편(33.3%), 5∼10주 사이가 6편이었고(28.5%), 2개월에서 6개월 후는 4편이었다(19.0%).
- 21편의 연구에서 적용한 수용전념치료의 중재 횟수는 8회기로 진행한 연구가 15편(71.4%), 10회기가 6편(28.6%)이었다. 수용전념치료에는 현재에 머무르기, 맥락적으로 이해하기, 수용, 인지적 탈융합, 가치 그리고 전념행동의 6가지 기본 원리가 있는데(Hayes & Lillis, 2012), 대부분의 연구에서 사용한 중재방법은 Moon(2006)이 제안한 수용전념치료 프로그램과 유사한 구성으로 6가지 기본원리를 연구의 목적에 따라 수정 보완한 것이었다. 즉, 매 회기의 도입부를 간단한 명상으로 시작하여 현재에 머무르기와 수용하기 연습을 진행하고, 경험의 통제와 회피방법의 비효율성을 자각하게 도와 창조적 절망감(creative hopelessness)을 이끌어내면서 변화의 동기를 이끌어내었다. 그 다음으로는 자신의 경험을 평가하거나 판단하지 않고 있는 그대로 보도록 하여 경험에 언어가 융합되지 않도록 하고(인지적 탈융합), 자신을 맥락적으로 파악하고 이해하며 삶의 방향을 제시하는 자신의 가치를 찾도록 도와주었다. 마지막으로 자신의 가치를 향한 전념행동을 하도록 계획을 세우고, 이를 방해하는 장애물이 무엇인지를 찾으며, 변화 가능한 영역 안에서 행동하도록 돕는 순서로 진행하였다. 21개의 연구 모두에서 수용전념치료의 6개 기본원리를 적용하는 진행순서는 유사하였으나 대상자의 특성과 중재의 목적에 따라 특정한 원리에 대한 추가 회기를 진행하였다.
- 3. 대상자에 따른 수용전념치료 중재의 내용과 효과
- 수용전념치료의 효과를 측정한 변수는 수용측정 도구, 증상관련 척도 및 심리적 문제를 측정하는 도구를 많이 사용하였는데 가장 많이 사용한 도구는 21개의 논문 중 13개의 논문(61.9%)에서 사용한 수용행동질문지(Acceptance and Action Questionnaire: AAQ)였다. 수용행동질문지는 심리적 건강의 지표인 심리적 유연성을 측정하는 도구이며, 역산하였을 때는 경험의 회피를 측정하는 도구로 사용될 수 있다. 이 도구를 사용한 13개의 논문에서 모두 수용전념치료가 불안이나 우울 그리고 중독 환자들의 증상을 호전시키는데 도움을 주었을 뿐만 아니라, 심리적 유연성을 증진시키거나 경험의 회피를 줄이는 데도 효과적임이 확인되었다(Table 2).
- Chronological summary of the reviewed papers
-
Exp: experimental, Cont: control, TAU-treatment as usual, n. s.: no significant, SAT: Speech Anxiety Thought, BAI: Beck Anxiety Inventory, ASI: Anxiety Sensitivity Inventory, AAQ: Acceptance & Action Questionnaire, SADS: Social Avoidance and Distress Scale, SFA: Self Focused Attention, SAS: Speech Anxiety Scale, BCPA: Behavior Checklist for Performance Anxiety, SAS1,: Self-assertive Scale, SUDS: Subjective Units of Discomfort Scale, SATI: Speech Anxiety Thoughts Inventory, FNE: Fear of Negative Evaluation Scale, IBT: Irrational Beliefs Test, PWBS: Psychological Well-Being Scale, DBT: Dysfunctional Beliefs Test, SISST: Social Interaction Self-Statement Test, SIAS: Social Interactive Anxiety Scale, KCAMS-R: Korean Version of the Cognitive and Affective Mindfulness Scale-Revised, RSQ: Rejection Sensitivity Questionnaire, ISA: Interaction Anxiousness Scale, SSES: Social Self-Efficacy Scale, SCS: Self-Compassion Scale, MAAS: Mindfulness Attention Awareness Scale, SSAS: Self-Rated Smartphone Addiction Scale for Adult, CES-D: Center for Epidemiologic Studies Depression Scale, SAPS_A: Smartphone Addiction Proneness Scale for Adults, SCRS: Self-Control Rating Scale, STAI: Spielberg Trait Anxiety Inventory, AUDIT-K: Korean version of Alcohol Use Disorder Identification Test, PDST: Problem Drinking Screening Test. SES1,: Alcohol Expectancy Scale, PSS: Perceived Stress Scale, ATQ-N: Automatic Thought Questionnaire-N, PANS: Positive Affect and Negative Affect Schedule, TSWLS: The Satisfaction with Life Scale, LOT: P: Revised Life Orientation Test, OES-A: Outcome Expectancy Scale-alcohol, AU: Alcohol Urge Questionnaire, MSA: Mood Awareness Scale, EMS: Emotional Expressiveness Scale, AEQ: Ambivalence over Emotional Expressiveness Questionnaire, CTQ: Childhood Trauma Questionnaire, CROPS: Child Report Of Post-traumatic Symptoms, ER: Ego-Resiliency Scale, IIP: Inventory of Interpersonal Problems, PTSD: Posttraumatic Stress Disorder, PTSDs: Posttraumatic Stress Diagnostic Scale, CPTSSs: Complex Posttraumatic Stress Symptoms Scale PTCI: Posttraumatic Cognitions Inventory, DERS: Difficulties in Emotion Regulation Scale, BET: Body Esteem Test, BCS: Body Cathexis Scale, K-BICSI-A: Korean- Body Image Coping Strategy Index- Avoidance, STAXI-K: Sate-Trait Anger Expression Inventory-Korean, EES: Emotional Eating Scale, K-CBCL: Child Behavior Checklist.
- 불안 대상자에게 수용전념치료를 적용한 논문은 8편이었고 세부 분류로 사회불안, 대인불안 및 발표불안 대상자였다. 불안 대상자들에게 수용전념치료를 적용한 연구들에서 사용한 중재는 공통적으로 인지적 탈융합 원리를 적용하는 회기를 늘려서 운영하여, 불안에 대한 인지적 영향을 감소시키고 원하지 않는 상황을 회피하지 않고 머무르게 하면서 전념행동을 하도록 유도하였다. 수용전념치료 후 대상자들의 상태불안, 특성불안, 불안 민감성 그리고 회피적인 반응은 감소되었으며 불안 통제감은 증가하였다.
- 발표불안을 가진 대학생에게 수용전념치료를 적용한 3개의 연구결과에서는, 개인이 지각한 발표불안, 우울, 불안 민감성, 주관적 불편감, 사회적 회피 그리고 자기 초점주의 성향이 감소하였으며, 심리적 유연성과 관련 있는 수용행동은 증가하는 결과를 보였다. 또한 불안이라는 감정을 있는 그대로 받아들이는 과정으로 통해 인지적 왜곡이 줄어들고 거절 민감성, 부정적 평가에 대한 공포, 비합리적 신념이 감소하고 심리적 안녕감은 증가했다. 그러나 중재 후 발표불안 사고의 빈도나 사고확신 점수에는 차이가 없는 것으로 보고되었다.
- 사회불안에 대한 인지행동치료(CBT)와 수용전념치료(ACT)의 효과를 비교 분석한 연구결과에서는 두 가지 중재 모두 프로그램 직후에 역기능적인 사고와 부정적 상호작용 자기 진술 그리고 수행불안이 감소하였다. 마음챙김과 수용행동은 수용전념치료군에서 인지행동치료군보다 중재 전후 차이가 많았으며 통계적으로도 두 집단이 유의한 차이가 있었고, 3개월 뒤에도 그 효과가 유지되는 것으로 보고 되었다. 수용전념치료군의 긍정적 상호작용 자기진술과 사회적 상호작용불안은 중재 직후 유의하지 않았으나 3개월 뒤 추적 조사에서 유의하게 증가하였다.
- 대인 불안을 가진 대상자에게 수용전념치료를 중재한 연구에서는 중재 후 상호작용 불안과 정서 중심의 대처가 감소하고 사회적 자기 효능감, 문제중심의 대처 그리고 수용행동이 증가하였음을 확인하였다.
- 우울 대상자에게 수용전념치료를 적용한 논문은 2편이었다. 우울대상자에게 적용한 수용전념치료에서는 마음 챙김을 통해 판단하지 않는 자기 수용을 강조하고 자신을 맥락적으로 이해하여 부정적인 자기반추를 줄이도록 도와 우울을 중재하였다. 두 편의 연구 모두에서 중재 후 대상자는 수용행동, 마음 챙김, 그리고 자기 자비와 같은 매개요인 점수가 높아졌고 우울수준이 감소되었다. 또한 자기 자비와 수용행동은 우울한 대상자의 심리적 유연성이나 심리적 안녕감을 증가시키고 자살사고 감소에 영향을 주는 것으로 나타났다.
- 중독 대상자에게 수용전념치료를 적용한 연구는 5편이었다. 이들에게 적용한 수용전념치료는 중독대상자가 가진 불안과 자신이 해왔던 통제나 회피 방법의 비효과성을 강조하는 내용으로 구성되었다. 회피방법보다는 자신들의 심리적 문제를 직면하고 수용할 수 있게 격려하며 스스로 정한 가치를 향한 전념 행동을 실행하게 하고 심리적 장애물을 극복하도록 도와주는 중재를 시행하였다. 스마트폰 중독 고위험군을 대상으로 한 연구에서는 수용전념치료 후 심리적 유연성과 자기조절이 증가하였으며 특성불안이 감소하였고 4주 뒤의 추적 조사에도 그 효과가 지속된다는 것을 확인하였다. 알코올 문제가 있는 대학생에게 수용전념치료를 중재한 연구에서는 문제 음주 행동과 알코올에 대한 기대 그리고 스트레스가 감소되었다. 특히 병동에 입원한 알코올의존 환자에게 수용전념치료를 적용한 연구에서는 중재 후 수용행동, 긍정적인 정서 그리고 자존감이 증가하였고 부정적 자동사고는 감소하였음을 보고하였다. 그러나 알코올 의존환자의 삶의 만족도와 부정적인 정서 및 음주 변화에 대한 기대에는 영향을 미치지 않는 것으로 확인되었다.
- 외상 후 스트레스 장애 대상자에게 수용전념치료를 적용한 논문은 3편이었다. 외상 후 스트레스 장애 대상자에게 수용전념치료는 과거의 외상에서 벗어나 현재에 존재하기를 강조하고 자신의 현재 상태 수용을 통해 자신을 맥락적으로 바라보고 이해하는 내용으로 진행되었다. 대인관계에서 상처를 받거나 아동기 트라우마를 경험한 대학생들에게 수용전념치료를 적용한 연구에서는 외상 후 스트레스 증후군, 복합외상 후 스트레스 증후군 증상 및 부정적인 인지가 감소되었고 심리적 유연성은 증가된다고 보고하였다. 트라우마를 경험한 대상자는 수용전념치료 중재 후에 정서인식, 정서표현 그리고 양가감정 표현이 증가되는 것을 확인하였다. 청소년 대상 연구에서는 특히 자존감과 자아탄력성이 증가하고 대인관계문제는 감소하는 효과를 보고하였다.
- 신체상 장애 대상자에게 수용전념치료를 적용한 논문은 2편이었다. 식이 장애나 신체상의 문제가 있는 여자 대학생에게 수용전념치료를 적용 시 먼저 현재 대처방법의 비효과성을 강조하면서 창조적인 절망감을 유발시키고 효과적인 대처방법을 찾도록 도와주는 순서로 진행되었다. 그리고 외모가 아닌 자신이 진정으로 원하는 가치를 찾아 전념행동을 실천하는 것에 중점을 두고 중재하였다. 수용전념치료 중재 후 자아 존중감과 분노통제전략이 증가하고 스트레스, 폭식, 회피대처전략 그리고 상태분노가 감소하였으나 특성분노에는 차이가 없는 것으로 보고되었다. 그 외에도 학교부적응 대상자에게 수용전념치료를 적용한 논문은 1편이 있었다. 학교 부적응 문제가 있는 중고등학생에게 수용전념치료를 적용 시에는 먼저 현재 행동의 비효과성으로 강조하여 창조적인 절망감을 유발하고 자신을 맥락적으로 이해하는 시간을 가졌다. 그리고 자기이해를 통해 자신이 진정으로 원하는 가치를 찾아 전념행동을 할 수 있도록 중재하였다. 중재 후 분노와 행동문제는 감소하고 자아 존중감이 증가하였고 추적 조사에서도 효과가 유지되었음을 보고하였다.
결과
| Target | Author | Research design | Subject (n) | Intervention (time/interval/number of session/period) | Variables | Measurement period | Results |
|---|---|---|---|---|---|---|---|
| Speech anxiety | Kim & Kim (2012) | RCT | University student (SAT>90), N=28 (Exp.=14, Cont.=14) | 120 min/2~3/wk/8/no comment | SAT, BAI, ASI, AAQ | Pre-post | Speech anxiety thought (SAT) (d=5.13, 95% CI: 3.59~6.68), Anxiety (BAI) (d=2.43, 95% CI: 1.46~3.41), Anxiety sensitivity (Tonarelli, Pasillas, Alvarado, Dwivedi, & Cancellare) (d=1.14, 95% CI: 0.34~1.94), Acceptance & Action (AAQ) (d=0.82, 95% CI: 0.05~1.59) |
| Kim & Son (2013) | RCT | University student (SADS>82, SFA upper 25%), N=20, (Exp=10, Cont.=10) | 120 min/1/wk/8/8 wks | SADS, SFA, SAS, AAQ | Per-post 1 m later | Social Avoidance & distress (d=0.35, 95% CI:-0. 53~1.23), Self-Focused Attention (d=0.95, 95% CI:0. 03~1.88), Speech Anxiety (d=1.04, 95% CI: 0.07~1.93), AAQ (group effect) (d=1.54, 95% CI: 0.55~2.55) ⟶Keep effect until F/U | |
| Kim & Back (2013) | Non-RCT | University student (SAS>100), N=38, (Exp=19, Cont.=19) | 90 min/1/wk/8/8 wks | SAS, SUDS, SATIAvoidance scale | Pre- post | Speech Anxiety (SAS) (d=0.78, 95% CI: 0.12~1.44), Subjective units of discomfort (SUDS) (d=0.67, 95% CI: 0.01~1.33), Speech Anxiety Thoughts (SATI): n. s., Avoidance scale (d=0.78, 95% CI: 0.12~1.44) | |
| Social anxiety | Kwon & Chung (2014) | RCT | University student (SADA>92, upper 15%), N=78(, Exp=40, Cont.=38) | 120 min/1/wk/10/ 10 wks | SADS, BDI, FNE, IBT, PWBS. | Pre-post 4 m & 6 m later | Social Anxiety and Distress (SADS) (d=3.78, 95% CI: 3.04~4.52), Depression (BDI) (d=5.12, 95% CI: 4.20~6.03), Fear of Negative Evaluation (FNE) (d=2.58, 95% CI: 1.98~3.18), Irrational Beliefs (IBT) (d=3.73, 95% CI: 2.99~4.47), a Psychological Well-Being (PWBS) (d=4.04, 95% CI: 3.27~4.82) ⟶Keep effect until F/U |
| Ko & Kim (2015) | RCT | University student (SADS>82), N=21, ACT=7, CBT=7, Cont.=7 | 120 min/2/wk/10/5 wks | SADS DBT, SISST, K-CAMS-R, AAQ, SIAS, BCPA, SIAS, SAS1, | Pre-post 3 m later | Dysfunctional thinking (DBT) (d=0.61, 95% CI: -0.26~1.48), Social interaction- negative thinking a (SISST) (d=0.48, 95% CI: -0.38~1.35), Social interaction-positive thinking (SISST) (n. s.), Performance anxiety (BCPA) (d=1.13, 95% CI: 0.20~2.05), Self-awareness (ASA1) (d=1.13, 95% CI: 0.20~2.05), Mindfulness (K-CAMS-R) (d=1.13, 95% CI: 0.20~2.05), Acceptance & action (AAQ) (d=1.03, 95% CI: 0.12~1.94) ⟶Keep effect until F/U, Social interactive anxiety (SIAS) (3 m F/U d=1.13, 95% CI: 0.20~2.05) | |
| Kim & Son (2016) | RCT | University student (SADS>82), N=16, Exp=8, Cont.=8 | 120 min,/2/wk/10/5 wks | SADS RSQ, AAQ | Pre-post 5 weeks later | The Social Avoidance and Distress (SADS) (d=2.38, 95% CI: 1.10~3.67), Rejection Sensitivity (RSQ) (d=1.44, 95% CI: 0.34~2.54), Acceptance Action (AAQ) (d=3.12, 95% CI: 1.67~4.59)⟶Keep effect until F/U | |
| Interpersonal anxiety | Kim & Son (2013) | RCT | University student (ISA: upper 25%), N=18, Exp=9, Cont.=9 | 120 min/2/wk/8/4 wks | IAS, SSES, AAQ, Ways of Coping Checklist, | Pre-post 5 weeks later | Interaction Anxiousness (IAS) (d=2.25, 95% CI: 1.07~3.44), The Ways of Coping (emotion-alleviative coping style, problem focused coping style) (d=2.42, 95% CI: 1.21~3.64), Social Self-Efficacy (SSES) (d=3.93, 95% CI: 2.34~5.51), Acceptance & Action (AAQ) (d=1.22, 95% CI: 0.21~2.22)⟶Keep effect until F/U |
| Anxiety | Lee & Ahn (2012) | Non-RCT | University student (interview: MINI-pluse), N=58, Exp=31, Cont.=27 | 120 min/1/wk/10/ 10 wks | BDI, STAI, AAQ, TSI, ASI-, ACQ-R | Pre- post 10 weeks later | State & Trait Anxiety (STAI) (d=0.63, 95% CI: 0.10~1.16), Thought Suppression & Anxiety Sensitivity (ASI-R) (d=0.6195% CI: 0.09~0.15), Acceptance & Action (AAQ-I) (d=1.48, 95% CI: 0.89~2.06), Anxiety Control (ACQ-R) (d=0.93, 95% CI: 0.38~1.47) ⟶Keep effect until F/U |
| Depression | Yang & Shin (2013) | Non-RCT | University student(BDI>10, SSI>9), N=18, Exp=9, Cont.=9 | 90 min/2~3/wk/8/ 3 wks | BDI, PWBS, AAQ, Scale for Suicidal Ideation. | Pre- post | Suicidal Ideation (d=0.74, 95% CI: -0.21~1.69), Psychological Well-Being (PWBS) (d=0.72, 95% CI: -0.23~1.68), Acceptance & Action (AAQ) (d=0.72, 95% CI: -0.23~1.68) ⟶Keep effect until F/U |
| Kim & Park (2014) | RCT | University women student (BDI>13, CES-D>16, HRSD>16), N=30 (Exp=15, Cont.=15) | 60 min/1/wk/10/ 10 wks | BDI, AAQ, SCS, MAAS | Pre-post 2 m & 4 m later | Depression (BDI) (d=0.95, 95% CI: -0.19~1.70), Acceptance & Action (AAQII) (d=1.26, 95% CI: 0.47~2.04), Self-compassion (SCS) (d=1.09 95% CI: 0.41~1.96)⟶Keep effect until F/U | |
| Smartphone addiction | Ha & Son (2016) | Non-RCT | University student, (SSAS>40, CES-D: upper 25% of data), N=16 (Exp n=8, Cont. n=8) | 90 min/2/wk/8/4 wks | SSAS, CES-D, AAQSCRS | Pre-post 6 weeks later | Smartphone addiction (SSAS), depression (CES-D), Acceptance & Action (AAQ), self-control (SCRS) posttest: n. s., but 6 weeks F/u: self-control (SCRS) (d=1.34, 95% CI: -0.25~2.42) |
| Yu & Son (2016) | RCT | University student SAPS-A>40, N=18 (Exp=9, Cont.=9) | 120 min/2/wk/8/4 wks | SAPS-A, SCRS, STAI, AAQ | Pre=post 4 weeks later | Self-Control (SCRS) (d=0.97, 95% CI: -0.00~1.95), trait Anxiety (STAI) (d=0.84, 95% CI: -0.11~1.81), AAQ-I(d=1.05, 95% CI: -0.14~2.14) ⟶Keep effect until F/U | |
| Problem drinking behavior | Joh & Son (2013) | RCT | University student(AUDIK-K>12, PDST>3), N=14 (Exp=7, Cont=7) | 120 min/2/wk/8/4 wks | AUDIT-K, PDST, SES1, PSS | Pre=post 4 weeks later | Problem drinking behavior (d=-2.22, 95% CI: -3.56~-0.89), Alcohol expectancy (d=-0.8, 95% CI: -1.89~0.28), Perceived stress (d=-0.47, 95% CI: -1.53~0.58) ⟶Keep effect until F/U |
| Alcohol dependence | Lee & Son (2013) | RCT | Patients in hospital (IQ>90), N=30 (Exp=15, Cont=15) | 90 min/1/wk/10/10 wks | PWBS, AAQ, ATQ-N | Pre-post 5 weeks later | Negative automatic thought (ATQ-N) (d=-0.92, 95% CI: -1.67~-0.16) ⟶Keep effect until F/U |
| Jeong & Lee (2014) | Non-RCT | Patients in hospital, (age:30~50 yr,) N=24 (Exp=12, Cont=12) | 90 min/2/wk/8/4 wks | AAQ, PANAS, SWLS, LOT-R, OES-A, AU, The Rosenberg Self-Esteem Scale, | Pre-post | Acceptance& action (AAQ) (d=0.93, 95% CI: 0.09~1.78), Positive affect (PANS) (d=0.48, 95% CI: -0.33~0.29), Self-esteem (SES) (d=0.87, 95% CI: -0.04~1.71), Drinking outcome expectancy (OES-A) (d=0.87, 95% CI: 0.03~1.71) But Life satisfaction, Negative effect, Life orientation test and Alcohol urge questionnaire: n. s. | |
| PTSD | Seo & Kim (2012) | RCT | University student (childhood abuse history (+)) N=18 (Exp=9, Cont=9) | 90 min/1/wk/8/8 wks | MAS, EMS, AEQ | Pre-post | Mood awareness (MAS) (d=1.68, 95% CI: 0.85~2.52), Emotional expressiveness (EMS) (d=0.91, 95% CI: 0.16~1.66), Ambivalence over emotional expressiveness (AEQ) (d=1.25, 95% CI: 0.47~2.03) |
| Noh & Son (2014) | RCT | Middle & high school student (childhood abuse history (+), CTQ: upper 20% of data), N=28 (Exp=14, Cont=14) | 60 min/?/8/no comment | CTQ, CROPS, SES, ER, IIP. | Pre-post 4 weeks later | Post-traumatic Symptoms (CROPS) (d=0.70, 95% CI: -0.06~1.46), Self-Esteem (SES), Time effect (d=0.66, 95% CI: -0.09~1.42), Ego-Resiliency (ER) (d=0.79, 95% CI: 0.02~1.56), Interpersonal Problems (IIP) (d=0.98, 95% CI:0. 20~1.77) ⟶Keep effect until F/U | |
| Joo & Son (2015) | RCT | University student (trauma (+) & PTSD scale >11) N=24 (Exp=12, Cont=12) | 120 min/2/wk/8/4 wks | PTSDs, CPTSSs, PTCI, DERS, AAQ | Pre-post 4 weeks later | Posttraumatic stress symptoms (PTSDs) (d=1.96, 95% CI: 0.99~2.94), Complex posttraumatic stress symptoms (CPTSSs) (d=2.105, 95% CI: 1.10~3.10), Negative cognition (PTCI) (d=2.39, 95% CI: 1.34~3.43), Acceptance & action (AAQ) (d=1.25, 95% CI: 0.37~2.12), ⟶Keep effect until F/U | |
| Negative body image | Choi & Son (2011) | RCT | Women, BMI 19-24, BCS<94 (upper 25% of data), N=18 (Exp n=9, Cont=9) | 90~120 min/2/wk/8/ 4 wks | BET, BCS, SES, K-BICSI-A | Pre-post 4 weeks later | Self-esteem (SES) (d=1.57, 95% CI: 0.51~2.63), Body Image Coping Strategy - Avoidance (K-BICSI –A) (d=1.97, 95% CI: 0.85~3.10) ⟶Keep effect until F/U |
| Binge eating | Song & Son (2011) | RCT | University women (BES>18), N=14 (Exp=7, Cont=70) | 90~120 min/1/wk/8/ 8 wks | STAXI-K, EESstress scale | Pre-post 4 weeks later | State anger (STAXI-K) (d=2.94, 95% CI: 1.43~4.56), Anger control (STAXI-K) (d=3.75, 95% CI: 2.01~5.49), Stress (d=2.52, 95% CI: 1.11~3.92), and Binge eating (EES) (d=2.27, 95% CI: 0.93~3.62), but Trait anger: n. s. ⟶Keep effect until F/U |
| School maladjustment | Jang & Son(2012) | RCT | Middle & high school student: STXI-K:upper30 & K-CBCL>65, N=24, (Exp=11, Cont=11) | 120 min/2/wk/10/ 5 wks | STAXI-K, SES, K-CBCL | Pre-post 10 weeks later | Anger (STAXI-K) (d=1.30, 95% CI: 0.42~2.18), Problematic behavior (K-CBCL) (d=3.40, 95% CI: 2.15~4.65), Self-esteem (SES) (d=1.62, 95% CI: 0.70~2.54) ⟶Keep effect until F/U |
1) 불안
2) 우울
3) 중독
4) 외상 후 스트레스 장애
5) 신체상 장애와 학교 부적응
- 본 논문은 국내 수용전념치료 중재 연구에 대한 통합적 고찰 결과를 바탕으로 국내 수용전념치료 연구의 방향과 프로그램 구성과 내용 및 효과를 살펴보고, 이를 근거로 국내 수용전념치료의 강점과 한계를 파악하고 치료 효과성과 임상의 유용성을 알아보고자 한다.
- 1. 국내 수용전념치료의 연구 방향과 제한점
- 우리나라에서 이뤄지고 있는 수용전념치료 중재 연구의 방향을 살펴보면, 연구대상자는 주로 10대 후반의 청소년과 대학생이었다. 청소년이나 대학생들은 정서적, 지적 성숙의 과도기에서 새로운 역할과 사회적 요구에 맞춰서 재구조화를 이루어 나가는 과정을 겪게 된다(Jo H, 2013). 더불어 이 시기에는 학업 및 또래집단 형성 등과 관련된 스트레스가 증가되면서 우울, 불안, 스트레스, 자살 사고 등 정신건강 문제가 급격하게 증가하고 있어(Mo SH et al., 2013), 이들을 대상으로한 연구가 많은 것이라고 본다. 또한 정신건강 문제뿐만 아니라 학령기 학생들의 학교생활적응이나 학습문제에 적용한 연구도 발표되고 있다. 그러나 정신과 질환을 진단받았거나 정신과 치료를 받고 있는 환자를 대상으로 한 연구는 매우 드물다. 본 연구에서 살펴본 문헌 21편중 19편은 정신과적인 진단을 받지 않은 일반인들 중에서 불안이나 우울과 같은 정신건강문제를 가진 고위험군을 대상으로 하였고 단 2편의 연구에서만 정신과에 입원해 있는 중독환자를 대상으로 연구를 진행하였다. 이는 국내에서 병원에 입원한 환자를 대상으로 연구를 진행하는데 제도적으로 여러 가지 제한점이 있기 때문이라고 여겨진다. 그러나 외국의 연구에서 수용전념치료는 정신건강문제를 가진 고위험군 뿐만 아니라 진단을 받은 우울증, 불안장애, 정신증 환자들에게 다양하게 연구되고 있으며, 병원에 입원한 환자에게 급성기 의학적인 치료가 끝난 뒤 수용전념치료를 적용하는 것은 환자의 능동적인 치료 참여를 유도하며 효과적인 증상치료뿐만 아니라 장기간 치료를 지속하는데 매우 중요한 역할을 할 수 있음이 보고되고 있다(Davis et al., 2015). 구체적으로 정신증 환자를 대상으로 한 연구에서는 중재 후 환청이나 왜곡된 사고가 감소하였으며 효과도 장기간 지속된다고 보고되고 있다(Bach et al., 2002; P. Bach et al., 2013; P. Bach et al., 2011; Bach et al., 2006). 증상이 심한 기분장애 환자에게 수용전념치료를 시행한 뒤 증상의 호전이 보인 것이 보고되었으며(Gaudiano, 2004), 그 외에도 우울과 불안 그리고 만성통증 등과 같은 다양한 정신과적인 문제와 신체적 문제에 효과적인 것이 보고되고 있다(Powers et al., 2009). 그러므로 국내에서도 병원에 입원한 정신증 환자와 지역사회 만성 정신질환자를 대상으로 수용전념치료를 적용하고 그 효과성을 검증하는 연구를 적극적으로 시도할 필요가 있다.
- 2. 국내 수용전념치료의 진행방식의 특성
- 수용전념치료 프로그램의 진행방식은 본 연구에서 살펴본 21편의 논문은 대부분 Moon HM(2006)이 개발한 프로그램과 유사하게 먼저 창조적인 절망감을 유발하여 변화 의제를 이끌어내고 자신의 가치에 대한 접근을 시도하는 방식으로 진행되고 있다. 반면 서양의 연구에서는 대상자가 자신이 원하는 가치가 무엇인지 찾는 작업을 먼저 진행하고, 현재에 머무르며 자신을 관찰하고 수용하는 시간을 가지는 순서로 진행되었다. 그리고 대상자로 하여금 자신이 원하는 가치를 향해 나아가는지를 살펴보고, 가치를 향한 전념행동을 하도록 돕는 방식으로 진행하기도 하였다(Bloy et al., 2006). 이러한 진행방식의 차이는 서양에서는 자기표현을 중시하는데 비해 자기표현을 최소화하는 경향을 가진 동양의 사고방식의 차이를 고려한 것이라고 본다(Lee SY, 2013). 자기 표현을 중시하는 서양의 문화에서 수용전념치료 프로그램을 중재할 때 대상자에게 자신이 중요하게 여기는 가치를 먼저 끌어내 참여를 증진시키는 반면, 동양인은 자기표현을 최소화하는 특성을 가지고 있어 자신의 가치를 먼저 찾기보다는, 문제해결을 위해서는 회피하거나 통제하는 방법이 효과적이지 않음을 알게 하여 창조적 절망감(Creative Hopelessness)을 이끌어내고 대상자가 스스로 변화의 동기를 찾아내도록 도와 참여를 증진시키는 방법을 사용하고 있는 것이라고 사료된다. 그러나 최근 들어 우리사회도 자기표현이 증가하고 서구적인 사고방식으로 전환하는 경향이 있어, 대상자의 연령과 특성에 따라서 먼저 가치 탐색에 접근해서 동기를 유발하는 진행방식을 적용하는 것도 고려해볼 수 있겠다. 또한 국내에서 수행된 대부분의 연구에서 적용한 진행방식은 Moon HM(2006)이 개발한 프로그램을 활용하고 있었다. 그러나 수용전념치료의 진행방식을 정하는 데에 있어서 서양과 동양의 사고방식이나, 기존의 개발된 프로그램을 단순하게 적용하기 보다는, 연구 대상자의 특성과 프로그램의 목적에 적합하도록 합리적인 근거를 가지고 진행하는 것이 중요하다고 본다.
- 3. 대상자에 따른 수용전념치료 중재 전략
- 본 연구결과를 바탕으로 하여 대상자의 특성을 고려한 수용전념치료의 중재전략을 제안하고자 한다. 불안을 주 문제로 가지고 있는 대상자는 불안에 대해 비수용적이거나 회피적인 경향을 가지고 있으며 불안에 대한 역기능적인 사고가 융합되어 있는 경우가 많다(Salters-Pedneault et al., 2004). 그러므로 불안대상자에게 수용전념치료를 중재 시에는 기꺼이 경험하기와 인지적 탈융합을 강조하는 것이 불안을 다루는데 중요한 역할을 하게 된다. 우울 대상자의 경우는 일반적으로 자신을 쓸모 없는 존재로 지각하고 부정적인 자기 판단을 하는 것이 문제가 된다(Luoma et al., 2012). 본 연구결과에서 우울대상자에게 수용전념치료를 중재할 때 자신을 맥락적으로 이해하고 수용하는 과정을 통해 자기 자비와 자기수용을 강조하는 것이 효과적임이 확인되었다. 또한 중독대상자는 문제상황에 대해 비효과적으로 대처하는 것이 가장 주요한 문제이다(Lee SY, 2013). 중독대상자를 위한 수용전념치료 중재전략은 먼저 자신의 심리적인 문제를 직면하고 수용하는 과정을 제공하고, 이를 통해 자신의 가치를 찾아 바람직한 방향으로 문제 해결하도록 도와주어야 한다. 특히 중독문제를 가진 대상자들의 반복적인 비효과적인 대처를 줄이기 위해 실제로 전념행동의 실천을 강조하는 것도 중요할 것이다. 외상 후 스트레스 장애 환자의 경우, 대부분이 자신의 힘든 과거 경험에서 빠져 나오지 못하는 것이 주 문제이기 때문에, 수용전념치료 중재전략은 현재에 존재하기를 강조함으로써 외상에서 벗어나 현재의 자신을 수용하도록 돕는 것이 필요하다. 본 연구결과에서 확인된 바에 따르면 이러한 중재전략은 현실 왜곡과 부정적 인지를 줄이고, 현재 자신의 정서를 인식하고 적절하게 표현하는데 도움을 주었다.
- 또한 연구결과 수용전념치료는 대상자의 우울뿐만 아니라 자살생각을 감소시키는 것으로 나타났는데, Park K(2011)의 연구결과에서 외상의 경험이 있는 사람들의 수용적 대처와 수용전념행동은 자살사고에 밀접한 영향을 미치는 것과 연관 지어 생각할 수 있다. 이 결과는 자살사고가 원치 않는 심리적인 경험을 회피하기 위한 하나의 수단이라는 이론과 관련이 있다(Luoma et al., 2012). 즉 심리적 유연성이 개인의 정신건강과 적응에 영향을 미치며 마음챙김과 심리적 수용은 자신의 문제를 평정심있는 마음으로 바라보고 매순간 충만한 삶을 살 수 있도록 적응적인 방법으로 대처하도록 돕게 된다. 따라서 부정적인 정서를 기꺼이 경험하고 수용하도록 돕는 수용전념치료는 개인의 변화에 대한 긍정적인 수용을 촉진함으로써 자살사고를 줄이고 자신의 가치를 향해 전념행동을 하도록 도와주게 된다. 이러한 과정은 수용전념치료가 자살 예방 프로그램으로 활용 가능함을 보여준다.
- 이처럼 대상자의 증상이나 질병의 특성과 프로그램의 목적에 따라 수용전념치료의 6개 기본원리에서 관련성 높은 부분을 강조하는 것은 프로그램 구성과 진행 시 매우 중요한 전략이 될 수 있다.
- 4. 수용전념치료 효과를 측정하는 주요 변수
- 수용전념치료의 효과를 측정한 변수를 살펴보면, 본 연구의 고찰 대상이 된 연구에서 가장 많이 사용한 것은 수용행동질문지(Acceptance and Action Questionnaire: AAQ)로 측정한 심리적 유연성이다. 심리적 유연성은 수용전념치료에서 제안한 개념으로서, 가치 있는 결과가 있을 때 혹은 목적이 있는 행동을 변화하거나 유지하면서 현재의 순간에 충분히 접촉하는 능력을 말한다(Hayes et al., 2012). 13개의 논문에서 모두 수용전념치료가 불안이나 우울 그리고 중독 환자들의 심리적 유연성을 증진시키거나 경험의 회피를 줄이는 매우 중요한 변수임을 보여주었다. 이러한 결과는 심리적 유연성이 수용전념치료의 중요한 개념일 뿐만 아니라 정신건강을 매개하는 중요한 변수가 될 수 있음을 시사한다.
- 또한 우울 대상자에게 수용전념치료를 적용한 효과를 파악할 때에는 심리적 유연성뿐만 아니라 마음챙김과 자기 자비가 효과에 영향을 미치는 중요한 매개변수임을 확인하였다. 이는 수용전념치료의 마음챙김 요소를 통해 우울증 환자가 스스로를 비난하고 부정적인 기억을 다시 반추하는 행동을 줄이고 내적 경험을 수용하고 순간의 경험으로 인식하는 것이 매우 중요함을 시사하는 것이다(Academic Mindfulness Interest Group, 2006).
- 심리적 안녕감도 수용전념치료의 효과를 측정하는 주요한 변수로 사용되고 있었다. 자아수용, 환경 지배력, 긍정적 대인관계, 자율성, 삶의 목적, 개인적 성장의 6개 하위척도로 구성된 심리적 안녕감(psychological well-being scale)도구를 4개의 연구에서 수용전념치료의 효과를 측정하는 변수로 사용하였다. 사회가 복잡해지면서 사회에서 생존하기 위한 다양한 전략을 세우게 되는데 그 결과의 불확실성으로 인한 정서적 불편감은 매우 증가하고 심리적 안념감은 감소되고 있다(Cosmides et al., 2000). 게다가 불안정한 상황에서 인간은 정서적 경험의 회피를 많이 하게 되고 결국 개인이 환경과 상호작용하는 것을 방해하게 되고 결과적으로는 더 높은 수준의 정서적인 불편감을 경험하게 된다(Salters- Pedneault et al., 2004). 즉 불안, 우울 그리고 정서적인 불편감을 경험하는 대상자에게 경험의 회피를 줄이는 것은 사회적 회피나 거절 민감성과 줄이고 상황을 기꺼이 경험하고 수용하게 하도록 하며 대인관계나 사회적인 기능을 향상시키는데 도움이 되는 것으로 여겨진다(Hayes et al., 2012). 따라서 대상자의 문제 특성과 프로그램의 목적이 이와 관련된 경우에는 심리적 안녕감 변수는 수용전념치료의 효과를 민감하게 평가할 수 있을 것이다.
- 본 통합적 문헌고찰 결과를 토대로 수용전념치료 프로그램을 구성 시 중요한 중재전략을 제안하고자 한다.
- 첫째, 반복적인 마음챙김 명상 훈련을 사용하는 중재전략은 현실감을 제공하는데 효과적일 것이다. 반복적인 마음챙김 명상은 몸과 마음을 편안하게 이완시켜줄 뿐만 아니라, 생각과 감정을 관찰하는 과정을 통해 상황을 왜곡하지 않고 있는 그대로 살펴볼 수 있게 도와주기 때문이다(Jung HK, 2004). 이러한 방법은 자신의 증상을 수용하지 못하고 비효율적인 회피전략을 사용하는 대상자에게 적용할 수 있는 유용한 접근법임을 시사하며, 외국에서는 수용전념치료가 정신질환자의 심리적 유연성과 현실감을 증진시키는데 효과적임이 보고되고 있다(Tonarelli et al., 2016; Öst, 2014). 본 연구에서 고찰한 21개의 연구에서도 모두 수용전념치료 중재 시 매 회기마다 마음 챙김 명상을 하였고 대상자들에게 호흡명상, 먹기 명상 그리고 바디 스캔과 같은 다양한 명상을 통해 신체감각을 집중하도록 하였으며, 지금-여기로 주의를 모으고 판단 없이 현실을 자각할 수 있도록 돕는 과정을 진행하였다. 이러한 과정은 우울하거나 불안한 대상자들에게 자신이 처한 상황을 왜곡하지 않고 있는 그대로 받아들이고 수용하게 되며, 심리적 유연성도 증진하게 돕는다. 즉 우울이나 불안에 대한 빈도나 확신이 줄어들었다고 하기보다는 상황을 수용함으로써 민감성을 감소시키며 결과적으로 불안이나 우울에 영향을 준 것으로 여겨진다. 또한 수용전념치료에서 활용하는 마음챙김명상은 처해진 상황을 객관적으로 판단하고 수용하도록 도와줌으로써 환자 스스로 행동변화의 동기를 유발하도록 작용하기 때문에 장기적인 효과를 기대할 수 있으며, 특히 이러한 측면에서 볼 때 만성적인 질환을 가지고 있는 대상자에게 매우 효과적일 것이다(Masuda et al., 2007).
- 둘째, 인지적 탈융합을 위하여 비유나 은유 전략을 활용할 것을 제안한다. 수용전념치료는 전체적인 맥락을 우선으로 하며 기능적으로 어떻게 행동했는지를 보는 기능적인 맥락주의와 관계구성이론(Relational Frame theory)을 기반으로 하고 있다(Bach et al., 2006). 즉 언어의 의미가 과도하게 구성되고 추상적인 관계가 형성됨으로써 인간의 행동이 언어의 영향을 많이 받는다는 것을 지적하고 있다(Bach et al., 2002). 이러한 배경하에 수용전념치료에서는 대상자가 언어의 영향을 덜 받게 하기 위해 지시적인 언어사용과 설명보다는 ‘구덩이에 빠진 사람’, ‘괴물과 줄다리기’, ‘흰곰 생각하지 않기’ 등과 같은 다양한 은유나 비유를 사용하여 프로그램을 진행한다. 이러한 은유나 비유는 대상자가 가지고 있는 불안에 대한 생각을 인지적으로 탈융합하도록 만들어,‘불안’이라는 언어가 가지는 부정적 인지와 역기능적인 사고를 줄이는데 많은 영향을 미치는 것으로 나타났다. 하지만 이러한 인지적 접근은 급성기 환자들의 경우 증상으로 인해 은유를 이해하지 못하고 오히려 상황을 왜곡해서 해석할 수 있기 때문에 대상자 선정 시 주의해야 할 점으로 여겨진다.
- 셋째, 수용전념치료의 효과는 기존 치료법에 비해 충분한 시간이 필요하다는 것을 고려해야 한다. Bach et al.(2002)의 연구에서 수용전념치료가 중재 직후 기존의 치료법에 비해 정신증을 가진 환자가 왜곡된 사고를 믿는 정도가 낮아지고 4개월 뒤 추후 측정에서는 빈도도 같이 낮아졌다는 보고하였다. 그리고 스마트폰 중독 고위험군과 사회불안 대상자 연구에서 수용전념치료 중재 직후에는 유의한 차이가 없었던 결과변수들이 각각 6주와 3개월 후 추적조사에서 통계적으로 유의한 차이를 보였다. 이는 마음챙김 명상을 포함한 수용전념치료의 효과는 단기간 내에 경험할 수 있는 것이 아니고 일상생활에서 반복적인 연습이 필요함을 시사하는 내용이다(Jung HK, 2004). 그러므로 수용전념치료 적용 시에는 대상자로 하여금 단기적으로 효과를 보이지 않을 수 있으며, 가능한 한 습관화가 될 수 있도록 충분한 시간을 가지고 배운 것을 반복 훈련하는 것이 필요함을 강조하는 것이 바람직하다. 그리고 이러한 반복 훈련은 스스로 왜곡된 사고에서 빠져 나와 현실감을 갖는 데 도움이 될 수 있으며 수용하는 과정을 통해 자신이 진정으로 원하는 가치를 찾아 전념행동을 하고 환자 스스로 변화에 대한 희망과 회복 태도 증진하게 되므로 매우 의미 있다고 할 수 있다. 수용전념치료는 치료효과가 단기간에 나타나지 않을 수 있으며 적정 기간의 교육과 중재가 필요하고 급성기 중증 환자를 중재하는 방법으로는 적합하지 않는 제한점을 가지고 있으나, 6개의 핵심 원리는 정신질환자에게 상황이나 문제를 왜곡하지 않고 있는 그대로 바라보도록 돕기 때문에, 증상이나 상황을 수용하고 가치 있는 삶을 살아가는데 매우 효과적인 중재방법이 될 수 있다.
- 게다가 수용전념치료는 자신의 증상을 회피하고 병을 수용하지 못하는 비효율적인 회피 전략을 가지고 있는 조현병이나 양극성 장애와 같은 주요정신질환자가 자신의 질병을 받아들이고 치료에 주도적으로 참여하도록 돕는 유용한 접근법이 될 가능성이 있다. 하지만 아직까지 국내에서는 입원한 정신질환자를 대상으로 시행한 연구가 매우 적은 실정이다. 본 연구 결과를 바탕으로 조현병이나 양극성 장애 등, 주요정신질환자 많은 병원에 입원한 환자를 대상으로 한 특성화된 수용전념치료 중재를 개발하고 이를 제공하여 그 효과를 검증하는 연구가 시행될 수 있기를 기대한다.
고찰
- Academic Mindfulness, Interest Group M, Academic Mindfulness Interest, Group M. 2006;Mindfulness-based psychotherapies:a review of conceptual foundations, empirical evidence and practical considerations. Aust N Z J Psychiatry. 40(4):285-294. .ArticlePubMed
- Bach PA, Hayes SC. 2002;The use of acceptance and commitment therapy to prevent the rehospitalization of psychotic patients:a randomized controlled trial. J Consult Clin Psychol. 70(5):1129doi:http://doi:10.1037//0022-006X.70.5.1129.ArticlePubMed
- Bach PA, Gaudiano BA, Hayes SC, et al. 2013;Acceptance and commitment therapy for psychosis:intent to treat, hospitalization outcome and mediation by believability. Psychosis. 5(2):166-174. doi:http://dx.doi.org/10.1080/17522439.2012.671349.Article
- Bach PA, Hayes SC, Gallop R. 2011;Long-term effects of brief acceptance and commitment therapy for psychosis. Behav Modif. 36(2):165-181. doi:http://doi:10.1177/0145445511427193.ArticlePubMed
- Bach PA, Gaudiano B, Pankey J, et al. 2006, Acceptance, Mindfulness, Values, and Psychosis: Applying Acceptance and Commitment Therapy (ACT) to the Chronically Mentally Ill. pp 93-116. San Diego: .
- Bloy S, Oliver JE, Morris E. 2011 Using acceptance and commitment therapy with people with psychosis:A case study. Clin Case Stud 10(5):347-359. doi:http://doi:10.1177/1534650111420863
- Cho MJ, Sung SJ, Shin S Y, et al. 2012;The epidemiological survey of mental disorders in Korea 2011. Ministry of Health and Welfare Research Report.
- Choi Y. Y, Son C. N. 2011;Effects of Acceptance and Commitment Therapy(ACT) on Body Image Esteem, Avoidance, and Self-Esteem of College Women with Negative Body Image. The Korean Journal of Health Psychology. 16(4):657-673. .Article
- Cosmides L, Tooby J. 2000;Evolutionary psychology and the emotions. Handbook of emotions. 2:91-115. .
- Davis M, Morina N, Powers M, et al. 2015;A meta-analysis of the efficacy of acceptance and commitment therapy for clinically relevant mental and physical health problems. Psychother Psychosom. 84(1):30-36. doi:https://doi.org/10.1159/000365764ArticlePubMed
- Eifert GH, Forsyth JP, Arch J, et al. 2009;Acceptance and commitment therapy for anxiety disorders:Three case studies exemplifying a unified treatment protocol. Cogn Behav Pract. 16(4):368-385. doi:http://doi.org/10.1016/j.cbpra.2009.06.001.Article
- Gaudiano BA. 2004, Acceptance and commitment therapy for psychiatric inpatients with psychotic symptoms. Drexel University; Philadelphia: .
- Ha J, Son C. 2016;Effects of Acceptance and Commitment Therapy(ACT) on Self-Control, Depression, and Smartphone Addiction Level in University Students with High level of Depression and Smartphone Addiction. Korean Journal of Psychology: Addiction. 1(1):1-16.
- Hayes SC, Lillis J. 2012;Acceptance and commitment therapy: American Psychological Association Washington, DC.
- Hwang SO, Park SH. 2010;The Effects of the Acceptance & Commitment Therapy Model on the Middle School Students’ Test-Anxiety. The Korean Journal of East West Science. 13(2):83-95.
- Jeong NR, Lee MK. 2014;Effects of Acceptance-Commitment Therapy (ACT) on Mental Health of Inpatients with Alcohol Dependence. The Korean Journal of Health Psychology. 19(4):909-930. .Article
- Jang S, Son C. 2012;Effects of Acceptance and Commitment Therapy(ACT) on Anger, Problematic Behavior and Self-Esteem of Adolescents in School Maladjustment. The Korean journal of clinical psychology. 31(4):1059-1076. .Article
- Jimenez DE, Bartels SJ, Cardenas V, et al. 2013;Stigmatizing attitudes toward mental illness among racial/ethnic older adults in primary care. Int J Geriatr Psychiatry. 28(10):1061-1068. doi:https://doi:10.1002/gps.3928.ArticlePubMedPMC
- Jo HY. 2013;A Study on the College Level Post-adolescents’s Consciousness of Social Situation and Identities. Journal of Adolescent Welfare. 15(2):367-393.
- Johansson H, Eklund M. 2006;Helping alliance and early dropout from psychiatric out-patient care. Soc Psychiatry Psychiatr Epidemiol. 41(2):140-147. doi:https://doi:10.1007/s00127-005-0009-z.ArticlePubMed
- Joh YJ, Son CN. 2013;Effects of Acceptance and Commitment Therapy(ACT) on Problem Drinking Behavior, Alcohol Expectancy, and Perceived Stress of the College Students with Problem Drinking. The Korean Journal of Health Psychology. 18(3):445-467. .Article
- Johns LC, Oliver JE, Khondoker M, et al. 2016;The feasibility and acceptability of a brief Acceptance and Commitment Therapy (ACT) group intervention for people with psychosis:The ‘ACT for life’ study. J Behav Ther Exp Psychiatry. 50:257-263. .ArticlePubMed
- Joo Sj, Son C. 2015;Effects of Acceptance and Commitment Therapy(ACT) on Posttraumatic Stress Symptoms and Complex Posttraumatic Stress Symptoms of College Students with Interpersonal Trauma. The Korean Psychological Association. 34(2):353-374.Article
- Kim DH, Son CN. 2016;Effects of Acceptance and Commitment Therapy(ACT) on Social Anxiety, Rejection Sensitivity and Acceptance of Social Anxiety Disorder-prone College Students. The Korean journal of clinical psychology. 35(1):101-119. .Article
- Kim H, Park K. 2014;The Effects of Process Variables in Acceptance Commitment Therapy for Women’s Depression. The Korean journal of clinical psychology. 33(3):429-460. .Article
- Kim HE, Kim DY. 2012;The Effects of Acceptance and Commitment therapy on Anxiety Thought, Anxiety Sensitivity, and Acceptive Attitude: Focused on Public Speaking Anxiety. The Korean Journal of Health Psychology. 17(2):299-310. .Article
- Kim JH. 2004;Types of Mindfulness Meditation and Their Implications for Cognitive Behavioral Therapy. Cogn Behav Pract. 4(2):27-44.
- Kim JH, Na HJ. 2016;Mediating Effect of Self-Efficacy in the Relationship between Internalized Stigma and Treatment Adherence of Community Dwelling Patients with Mental Illness. J Korean Acad Psychiatr Ment Health Nurs. 25(1):11-20. doi:https://doi.org/10.12934/jkpmhn.2016.25.1.11Article
- Kim MO, Son CN. 2013;Effects of Acceptance and Commitment Therapy on Interpersonal Anxiety, Stress Coping Style, and Social Self-Efficacy of College Students with Interpersonal Anxiety. The Korean Journal of Health Psychology. 18(2):301-324. .Article
- Kim SI, Back JS. 2013;The Effects of Acceptance-Commitment Group Therapy on College Students’ Speech Anxiety Based on Cognitive Defusion Techniques. Korean journal of counseling and psychotherapy. 2(25):1. 19-40.
- Kingston J. 2008, Acceptance and commitment therapy (ACT) process and outcome: A systematic evaluation of ACT for treatment resistant patients. (Doctoral dissertation). University of Southampton; Southampton.
- Ko YJ, Kim JM. 2015;The Effect of Cognitive Behavioral Therapy and Acceptance and Commitment Therapy on Female University Students with Social Anxiety Disorder. Korea Society for the Emotional & Behavioral Disorders. 31(2):175-197.
- Kwon S, Chung H. 2014;Effects of the Acceptance and Commitment Therapy Program on Psychological Adjustment of University Students with a High Level of Social Anxiety. Cognitive Behavior Therapy in Korea. 14(2):145-164.
- Lee JH, Son CN. 2013;The Effects of the Acceptance-Commitment Group Therapy (ACT) on the Self-Control, Psychological Well-Being, Experiential Avoidance and Cognitive Fusion in Alcoholics. The Korean journal of stress research. 21(1):41-50.
- Lee OJ, Kim HS. 2004;A Study on Rehabilitation Program and Satisfaction for the Mental Health Disorders in the Residential Facilities. [A Study on Rehabilitation Program and Satisfaction for the Mental Health Disorders in the Residential Facilities]. J Korean Acad Psychiatr Ment Health Nurs. 13(4):449-457.
- Lee SY. 2013 Prevalence of conflicts and social pathologies at individual level and counter measures in Korea Available from http://www.riss.kr/link?id=E1053271
- Lee SY, Ahn CY. 2012;The Process Variables of Acceptance-Commitment Group Therapy for Anxiety and Effect. Korean journal of counseling and psychotherapy. 24(2):223-254.
- Luoma JB, Villatte JL. 2012;Mindfulness in the treatment of suicidal individuals. Cogn Behav Pract. 19(2):265-276. doi:https://doi.org/10.1016/j.cbpra.2010.12.003ArticlePubMed
- Masuda A, Hayes SC, Fletcher LB, et al. 2007;Impact of acceptance and commitment therapy versus education on stigma toward people with psychological disorders. Behav Res Ther. 45(11):2764-2772. doi:http://doi:10.1016/j.brat.2007.05.008.ArticlePubMed
- Mo SH, Kim HJ, Lee SY, et al. 2013;Improve actual children·adolescents’ mental health promotion through the development mental health promotion program for field application III: final Report. Korea Youth Policy Institute Research Report. 1-338.
- Moon HM. 2005;The Third Wave of Cognitive-Behavioral Therapy. The Korean Journal of Counselling and Psychoterapy. 17(1):15-33. .
- Moon HM. 2006 Development and validation of the program for facilitation of psychological acceptance based on acceptance & commitment therapy model. Doctoral dissertation The Catholic University of Korea; Seoul, Available from http://www.riss.kr/link?id=T10522732
- Noh PR, Son C. 2014;Effects of Acceptance and Commitment Therapy (ACT) on Self-Esteem, Interpersonal Problem, and Ego esilience of Adolescent with Childhood Trauma. The Korean Journal of Health Psychology. 19(4):885-910. .
- Öst LG. 2014 The efficacy of acceptance and commitment therapy:an updated systematic review and meta-analysis. Behav Res Ther 61:105-121. doi:http://dx.doi.org/10.1016/j.brat.2014.07.018ArticlePubMed
- Park K. 2011;The Relationship between Acceptance, Posttraumatic Growth, Depression, and Suicidal Ideation. The Korean journal of stress research. 19(4):281-292.
- Powers MB, Zum Vörde, Sive Vörding MB, Emmelkamp PM. 2009;Acceptance and commitment therapy:A meta-analytic review. Psychother Psychosom. 78(2):73-80. doi:https://doi.org/10.1159/000190790ArticlePubMed
- Salters-Pedneault K, Tull MT, Roemer L. 2004 The role of avoidance of emotional material in the anxiety disorders. Appl Prev Psychol 11(2):95-114. doi:http://doi.org/10.1016/j.appsy.2004.09.001Article
- Seo MJ, Kim DY. 2012;The Effects of Acceptance and Commitment Therapy on Emotional Identification, Emotional Expressiveness and Negative Belief of University Students with an Experience of Childhood Emotional Abuse. The Korean Journal of Health Psychology. 17(3):557-572. .Article
- SIGN. 2015;The Scottish intercollegiate guidelines network (SIGN) -(1).
- Song HJ, Son CN. 2011;The Effects of Acceptance and Commitment Therapy on Anger, Stress, and Binge Eating Behaviour of the Binge Eating Disorder-prone College Students. The Korean Journal of Health Psychology. 16(1):15-27. .Article
- Tonarelli S, Pasillas R, Alvarado L, et al. 2016;Acceptance and Commitment Therapy Compared to Treatment as Usual in Psychosis:A Systematic Review and Meta-Analysis. J Psychiatry. 19(366):2doi:http://dx.doi.org/10.4172/2378-5756.1000366.Article
- Yang SY, Shin HK. 2013;Effects of Acceptance and Commitment Therapy on Psychological Acceptance, Psychological Well-being, Depression and Suicidal Ideation of Depressed College students. The Korean journal of clinical psychology. 32(4):761-782. .Article
- Yu HG, Son C. 2016;Effects of ACT on Smartphone Addiction Level, Self-Control, and Anxiety of College Students with Smartphone Addiction. Journal of Digital Convergence. 14(2):415-426. doi:http://doi.org/10.14400/JDC.2016.14.2.415.Article
References
Figure & Data
References
Citations

- Psychometric properties of the Psy-flex scale: A validation study in a community sample in Korea
Duckhyun Jo, Byeori Seong, Eunjoo Yang
Journal of Contextual Behavioral Science.2023; 30: 70. CrossRef - The Effect of a Job Stress Management Program Based on Acceptance-Commitment Therapy for Firefighting Paramedics
Jae Woon Lee, Jae-Hyun Ha
Journal of Korean Academy of Fundamentals of Nursing.2021; 28(1): 56. CrossRef - Effects of Acceptance Commitment Therapy Based Recovery Enhancement Program on Psychological Flexibility, Recovery Attitude, and Quality of Life for Inpatients with Mental Illness
In Sook Kim, Jae Woon Lee
Journal of Korean Academy of Psychiatric and Mental Health Nursing.2019; 28(1): 79. CrossRef - The Relationship between the Decentering and Forgiveness: The Moderating Effect of Reflective Response Style and the Mediating Effect of Anger Rumination
Jiwon Shin, Youngho Lee
Stress.2019; 27(1): 36. CrossRef - Mediating Effect of Psychological Flexibility on Quality of Life in Inpatients with Schizophrenia
Hyun Sook Park, Jae Woon Lee
Journal of Korean Academy of Psychiatric and Mental Health Nursing.2018; 27(3): 284. CrossRef - The Effects of an Acceptance-Commitment Therapy Based Stress Management Program on Hospitalization Stress, Self-Efficacy and Psychological Well-Being of Inpatients with Schizophrenia
Jae Woon Lee, Jae Hyun Ha
Journal of Korean Academy of Nursing.2018; 48(4): 443. CrossRef - Improving Diabetes Self-Mangement and Mental Health through Acceptance and Commitment Therapy
Sung-Chul Lim
The Journal of Korean Diabetes.2018; 19(3): 186. CrossRef - Development and Effects of an Acceptance Commitment-based Cognitive Behavioral Program for Patients with Schizophrenia
Jae Woon Lee, Hyun Sook Park
Journal of Korean Academy of Psychiatric and Mental Health Nursing.2018; 27(4): 342. CrossRef - Mediating Effect of Depression on the Relationship between Gambling Severity and Cognitive Distortion: Secondary Data Analysis of Korea Center on Gambling Problems
Keelyong Lee, Jungah Hong
Journal of Korean Academy of Psychiatric and Mental Health Nursing.2018; 27(4): 370. CrossRef


 PubReader
PubReader Cite
Cite
